A friend of mine adopted a white Bichon Frise two years ago. Beautiful dog, absurd personality, and within three months, those telltale rusty streaks running from the inner corners of both eyes down to the muzzle. She tried everything the internet suggested: coconut oil, apple cider vinegar rinses, switching to filtered water. Some of it helped marginally. Most of it didn’t.
What eventually made a difference was understanding that tear staining is a symptom, not a standalone problem. The stain itself is just the visible residue of a process that begins with tear chemistry, facial anatomy, and microbial activity. Once you address the upstream causes rather than scrubbing at the downstream evidence, the situation changes.
This guide walks through the science of tear staining, the breeds most predisposed to it, and a practical framework combining external care with internal supplementation.
What causes tear stains, exactly?
The reddish-brown discoloration in tear stains comes primarily from a compound called porphyrin. Porphyrins are iron-containing molecules produced during the normal breakdown of red blood cells, and they’re excreted through tears, saliva, and urine (Gelatt et al., 2013). When tears sit on facial hair and are exposed to sunlight, the porphyrins oxidize and darken, producing that characteristic rust color.
But porphyrin alone doesn’t explain why some animals stain heavily and others don’t. Several factors determine severity:
Epiphora: excessive tear production or poor drainage
The medical term for excessive tearing is epiphora. It can result from overproduction (the eye makes too many tears) or from impaired drainage (the nasolacrimal duct, which normally channels tears from the eye into the nasal cavity, is blocked or underdeveloped).
In brachycephalic breeds like Shih Tzus, Pugs, and Persian cats, the shallow eye sockets and compressed facial anatomy physically distort the nasolacrimal duct pathway. Tears overflow onto the face rather than draining internally (Maggs et al., 2013).
Bacterial and yeast overgrowth
The warm, moist environment created by chronic tearing is hospitable to microorganisms. Malassezia yeast and certain bacterial species thrive in this environment, and their metabolic byproducts can intensify discoloration. This is why tear stains sometimes appear more red-brown than the pinkish hue of porphyrin alone (Petersen-Jones & Crispin, 2002).
Diet and water mineral content
High iron content in drinking water or food can increase porphyrin levels in tears. Some owners report improvement after switching to distilled or reverse-osmosis filtered water, though controlled studies on this specific intervention in companion animals are limited.
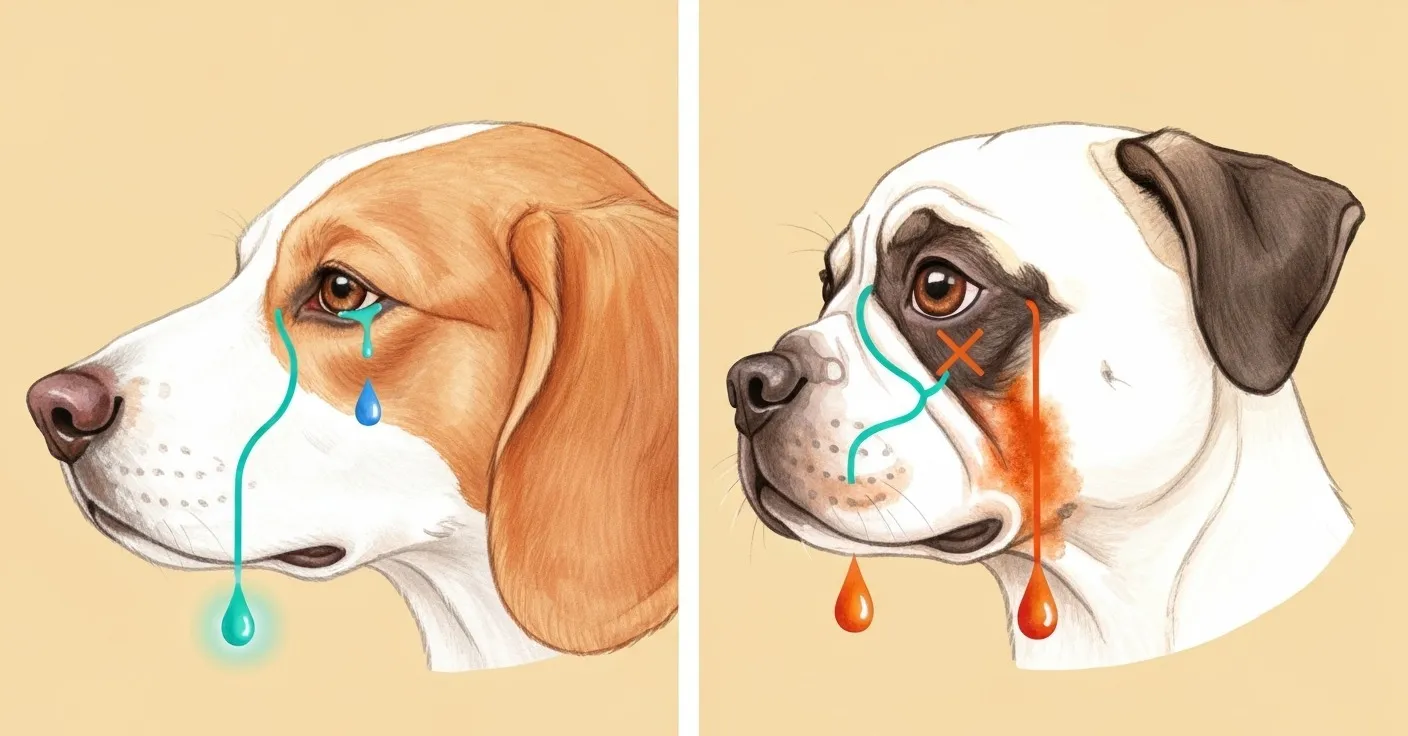
Left panel: teal line traces the nasolacrimal duct draining cleanly to the nostril in a normal-anatomy dog. Right panel: kinked, blocked duct in a flat-faced breed — orange overflow tears cascade down the muzzle, leaving rust-brown staining on the fur.
Which breeds are most prone to tear staining?
Tear staining has a strong breed predisposition. If you own one of these breeds, you’re not imagining it, and you’re not doing anything wrong.
Dogs
| Breed | Primary Risk Factor |
|---|---|
| Maltese | White coat amplifies visibility; shallow nasolacrimal anatomy |
| Bichon Frise | Dense facial hair traps moisture; prominent eyes |
| Shih Tzu | Brachycephalic skull; duct obstruction common |
| Poodle (Toy & Miniature) | Light coat colors; genetic predisposition to epiphora |
| Cocker Spaniel | Eyelid conformation issues; entropion risk |
Cats
| Breed | Primary Risk Factor |
|---|---|
| Persian | Extreme brachycephaly; chronic epiphora almost universal |
| Himalayan | Persian-derived facial structure |
| Exotic Shorthair | Brachycephalic; similar duct anatomy to Persians |
| Scottish Fold | Eye shape and facial structure contribute |
Light-colored coats don’t cause more staining; they just make existing staining dramatically more visible. A black Labrador produces porphyrins at comparable levels, but you’ll never see the evidence against dark fur.
External management: the daily routine
No supplement or dietary change eliminates the need for daily face care in stain-prone breeds. Think of external management as damage control while internal strategies address root causes.
Step 1: Morning wipe
Use a soft, damp cloth or a pet-specific eye wipe to clean the area below and around the eyes each morning. This removes overnight tear accumulation before porphyrins have time to oxidize and set into the fur.
A few principles matter here:
- Wipe outward, away from the eye, to avoid pushing debris toward the cornea.
- Don’t use hydrogen peroxide or bleach-containing products near the eyes. The mucous membranes are fragile, and chemical burns happen faster than you’d expect.
- Dry the area after wiping. Residual moisture perpetuates the problem.
Step 2: Keep facial hair trimmed
Long hair around the eyes acts as a wick, drawing tears laterally across the face and increasing the stained surface area. Regular trimming minimizes contact time between tear fluid and fur.
Step 3: Monitor for secondary infection
If the stained area develops a foul odor, becomes red and irritated (beyond the stain color), or if your pet is pawing at the face, schedule a veterinary visit. These signs suggest yeast or bacterial overgrowth that may require topical antifungal or antibiotic treatment.

Internal strategies: addressing stains from the inside
This is where most pet owners hit a wall. External cleaning manages the symptom, but if the tear chemistry, microbial balance, or inflammatory state driving the staining isn’t addressed, you’re on a treadmill.
Several evidence-informed internal approaches deserve attention:
Lactoferrin: antimicrobial and iron-binding
Lactoferrin is a glycoprotein naturally present in tears, saliva, and milk. It binds free iron, which serves two purposes in the context of tear staining: it reduces the iron available for porphyrin-related discoloration, and it deprives iron-dependent bacteria and yeast of a growth nutrient (Giansanti et al., 2016).
A study published in BioMetals demonstrated that lactoferrin exhibits broad-spectrum antimicrobial activity against both gram-positive and gram-negative bacteria, as well as against Candida species (Farnaud & Evans, 2003). When supplemented orally, lactoferrin may help modulate the microbial environment around the eyes by altering tear composition.
Lutein and eye-supportive antioxidants
Lutein is a carotenoid concentrated in the macula and lens of the eye. While it’s better known for its role in protecting against oxidative damage in human vision research, animal studies have shown that dietary lutein supplementation increases serum and tissue antioxidant capacity in dogs (Kim et al., 2000).
The relevance to tear staining is indirect but logical: oxidative stress can contribute to inflammatory processes in the periocular tissue, and reducing local inflammation may improve the integrity of the nasolacrimal drainage system.
Probiotics and gut-mediated immune support
The gut-eye axis is an emerging area of research. Systemic inflammation originating from gut dysbiosis can manifest in seemingly unrelated areas, including the eyes. A balanced gut microbiome supports appropriate immune regulation, which in turn may reduce the chronic low-grade inflammation that contributes to excessive tearing in some animals.
Lactobacillus strains have been shown to modulate systemic cytokine profiles in companion animals (Benyacoub et al., 2003), and this immunomodulatory effect could theoretically reduce the inflammatory component of epiphora.
For a deeper look at how probiotics support cats and dogs beyond digestion, see our article on probiotics for cats: 7 benefits beyond digestion.
L-Lysine and L-Threonine
Both amino acids play supporting roles. L-Lysine is widely included in feline eye-support formulas; research has explored its proposed role in supporting normal immune response in cats managing feline herpesvirus (FHV-1), which is linked to ocular discharge and secondary tear staining in some felines (Maggs, 2005). L-Threonine is a precursor to mucin production, which contributes to the stability of the tear film.
A combined internal approach
Supporting tear-area health effectively generally involves covering several pathways at once: antimicrobial balance, iron binding, antioxidant status, and gut-mediated immune support. That’s the rationale behind combination formulas rather than single-ingredient supplements.
Petterm’s Tear Stain Powder was formulated around this multi-pathway principle. Each sachet contains lactoferrin (60 mg), lutein (50 mg), Lactobacillus probiotics (6 billion CFU), L-Lysine (100 mg), oregano phenolics (20 mg), and vitamins A, E, B1, and B6. The powder format mixes into food, which tends to be more practical than eye drops for daily use, especially with cats.
It’s worth emphasizing that internal supplementation takes time. Most owners who report visible improvement describe a timeline of four to eight weeks of consistent daily use before new hair growth comes in unstained. The existing stained fur needs to grow out and be trimmed away.
Final thoughts
Tear staining frustrates owners partly because it looks like a grooming failure when it’s actually a physiological process. The stains are evidence of tear chemistry meeting facial anatomy, and in susceptible breeds, no amount of external wiping alone will eliminate them entirely.
A realistic approach combines consistent daily face care with internal supplementation that supports the upstream drivers: microbial balance, iron metabolism, antioxidant status, and immune regulation. It takes patience, a good four-to-eight-week commitment, and the understanding that you’re growing new unstained fur, not erasing existing stains.
If your pet’s staining is accompanied by discomfort, discharge changes, or sudden onset, that’s a veterinary visit rather than a supplement conversation. For the vast majority of cases, though, the combination of smart grooming habits and an evidence-informed supplement routine makes a meaningful difference.
Frequently asked questions
Do tear stain supplements actually work?
The individual ingredients in well-formulated supplements, including lactoferrin, lutein, and probiotics, have supporting evidence for their respective mechanisms. However, large-scale randomized controlled trials specifically measuring tear stain reduction in companion animals are limited. The best available evidence comes from mechanistic studies and clinical observations reported by veterinary dermatologists.
How long until I see results?
Expect four to eight weeks of daily supplementation before new, unstained hair growth becomes apparent. The existing stained fur won’t change color; it needs to grow out and be trimmed.
Is tear staining in cats different from dogs?
The underlying chemistry is the same (porphyrin oxidation), but the contributing factors differ somewhat. Cats, particularly Persians, are more likely to have congenital nasolacrimal duct stenosis. Cats are also more susceptible to herpesvirus-related ocular discharge, which adds an infectious component. Petterm Tear Stain Powder includes L-Lysine partly for this reason.
Can I use the same product for my dog and cat?
If the product is labeled for both species and provides dosing guidelines for each, yes. The Petterm Tear Stain Powder offers weight-based dosing for pets ranging from under 10 lbs to over 22 lbs, covering both small breed dogs and cats.
Does filtered water really help?
Anecdotally, many owners report improvement. The hypothesis is that high mineral content, particularly iron, in tap water increases porphyrin levels. Controlled studies are lacking, but switching to filtered water is low-cost and low-risk. It’s reasonable to try alongside other interventions.
When to contact your veterinarian
Not all tear staining is benign. A supplement routine is a long-term support tool, not a replacement for veterinary evaluation when something looks off.
Watch and support at home if: staining is mild, bilateral, chronic, and unchanged in pattern. The eyes themselves look clear and comfortable.
Call your vet within 24–48 hours if: staining appears suddenly in an adult pet, affects only one eye, is paired with squinting or head shyness, or the skin under the stain becomes red, thickened, or foul-smelling.
Seek veterinary care the same day if: you see green or yellow discharge, cloudiness, visible corneal damage, swelling around the eye or muzzle, or your pet is pawing at the face persistently. These signs warrant diagnostic workup that may include a Schirmer tear test, fluorescein staining to check for corneal damage, or nasolacrimal duct flushing (Maggs et al., 2013).
References
-
Gelatt, K.N., Gilger, B.C., & Kern, T.J. (2013). Veterinary Ophthalmology. 5th ed. Wiley-Blackwell.
-
Maggs, D.J., Miller, P.E., & Ofri, R. (2013). Slatter’s Fundamentals of Veterinary Ophthalmology. 5th ed. Elsevier.
-
Petersen-Jones, S. & Crispin, S. (2002). BSAVA Manual of Small Animal Ophthalmology. 2nd ed. BSAVA.
-
Giansanti, F., et al. (2016). “Lactoferrin from milk: nutraceutical and pharmacological properties.” Pharmaceuticals, 9(4), 61.
-
Farnaud, S. & Evans, R.W. (2003). “Lactoferrin: a multifunctional protein with antimicrobial properties.” Molecular Immunology, 40(7), 395-405.
-
Kim, H.W., et al. (2000). “Dietary lutein stimulates immune response in the canine.” Veterinary Immunology and Immunopathology, 74(3-4), 315-327.
-
Benyacoub, J., et al. (2003). “Supplementation of food with Enterococcus faecium (SF68) stimulates immune functions in young dogs.” Journal of Nutrition, 133(4), 1158-1162.
-
Maggs, D.J. (2005). “Update on pathogenesis, diagnosis, and treatment of feline herpesvirus type 1.” Clinical Techniques in Small Animal Practice, 20(2), 94-101.
Written by Dr. Liam Carter, Canine & Feline Wellness Advisor · Last reviewed April 2026
This article is for educational purposes and is not veterinary medical advice. Petterm products are not intended to diagnose, treat, cure, or prevent any disease. Results may vary. Always consult your veterinarian before introducing a new supplement, especially if your pet has an existing eye condition, takes medication, is pregnant, or is under 12 weeks old.
